 9 rapid decision algorithms at a glance — edema workup through metabolic acidosis correction. Each pathway distills KDIGO 2024, ACC/AHA, and local DOH guidance into outpatient-ready clinical steps.
9 rapid decision algorithms at a glance — edema workup through metabolic acidosis correction. Each pathway distills KDIGO 2024, ACC/AHA, and local DOH guidance into outpatient-ready clinical steps.
Outpatient Edema Workup
Bilateral pitting edema is among the most common outpatient presentations. Identify the mechanism before prescribing diuretics.
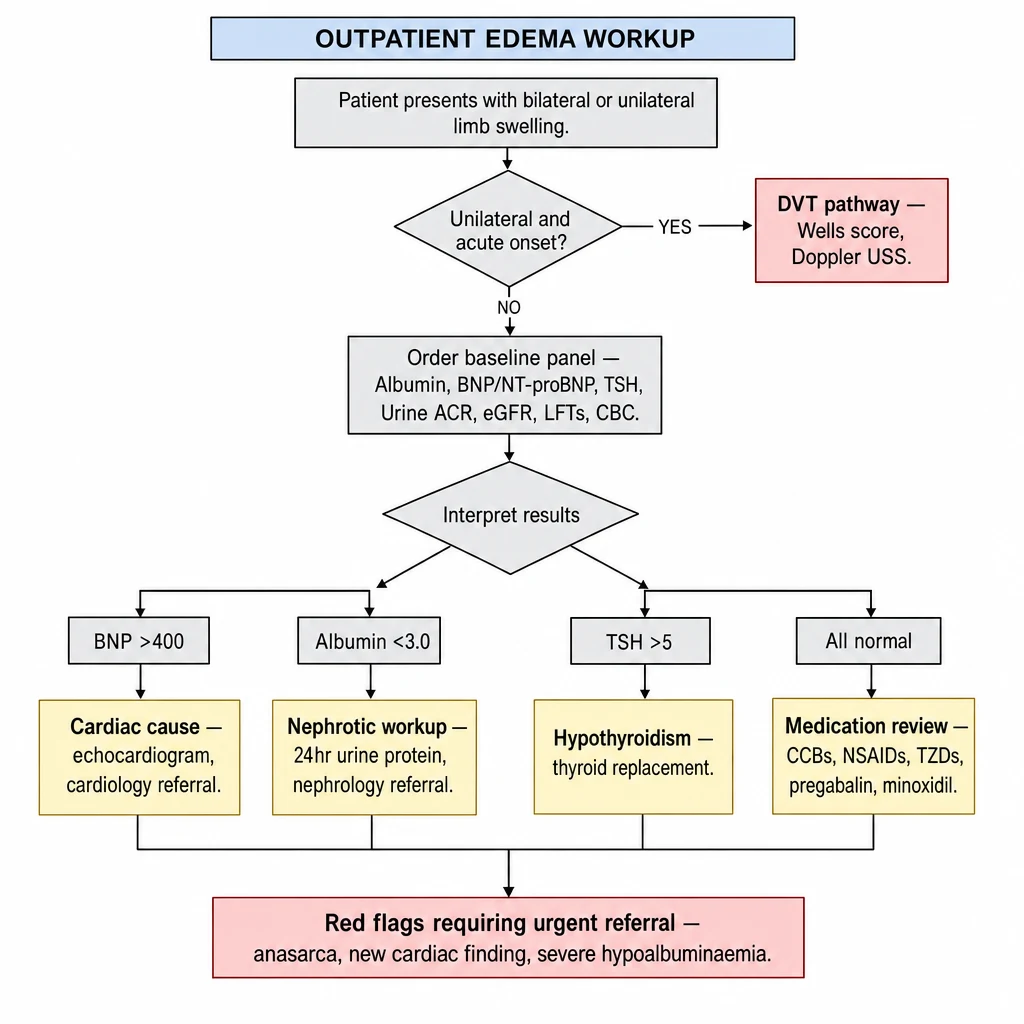 Algorithm 1 overview — Edema Workup. Begin with unilateral vs bilateral; order the targeted panel (BNP, albumin, TSH, ACR, eGFR); branch to cardiac, nephrotic, thyroid, or drug-induced cause. Anasarca or new cardiac finding = urgent referral.
Algorithm 1 overview — Edema Workup. Begin with unilateral vs bilateral; order the targeted panel (BNP, albumin, TSH, ACR, eGFR); branch to cardiac, nephrotic, thyroid, or drug-induced cause. Anasarca or new cardiac finding = urgent referral.
Apply Wells DVT score. If ≥2 points or high clinical suspicion → bilateral compression Doppler USS same day. If negative and score low → consider cellulitis, Baker's cyst ruptured, compartment syndrome, lymphedema (non-pitting, rubbery).
Bilateral edema almost always has a systemic cause. Proceed with mechanism-based workup.
Vitals review: BP, weight trend, O₂ saturation
Cardiac cause likely. Request echo. Refer cardiology if new finding. Optimise loop diuretic (furosemide). Check electrolytes and renal function.
Hypoalbuminaemia. Check urine protein (nephrotic if >3.5 g/day). Check LFTs for cirrhosis. Check total protein + SPEP if myeloma suspected. → Refer nephrology if nephrotic range.
Hypothyroid edema. Classic non-pitting myxedema. Start levothyroxine; edema resolves with euthyroid state over weeks.
Withdraw or switch offending agent. CCB-induced edema: switch to ARB + thiazide combination. Monitor for resolution over 2–4 weeks.
Most common in chronic bilateral ankle edema without systemic cause. Confirm with venous duplex. Manage: compression stockings, leg elevation, sodium restriction.
Quick Reference — edema Mechanism Map
- Increased hydrostatic pressure: CHF, venous insufficiency, hypoalbuminaemia
- Decreased oncotic pressure: nephrotic syndrome, cirrhosis, malnutrition
- Increased capillary permeability: inflammation, allergy, infection
- Lymphatic obstruction: lymphedema (non-pitting), filariasis
- Sodium/water retention: CKD, medications, SIADH
- Tip: Amlodipine is the most missed cause in the Philippines — always check CCB use first
Hyperkalemia Management
Outpatient-focused. Any K⁺ ≥ 6.0 mEq/L requires an ECG before a management decision. Type IV RTA (hyporeninaemic hypoaldosteronism) is the most common cause in CKD/DKD outpatients.
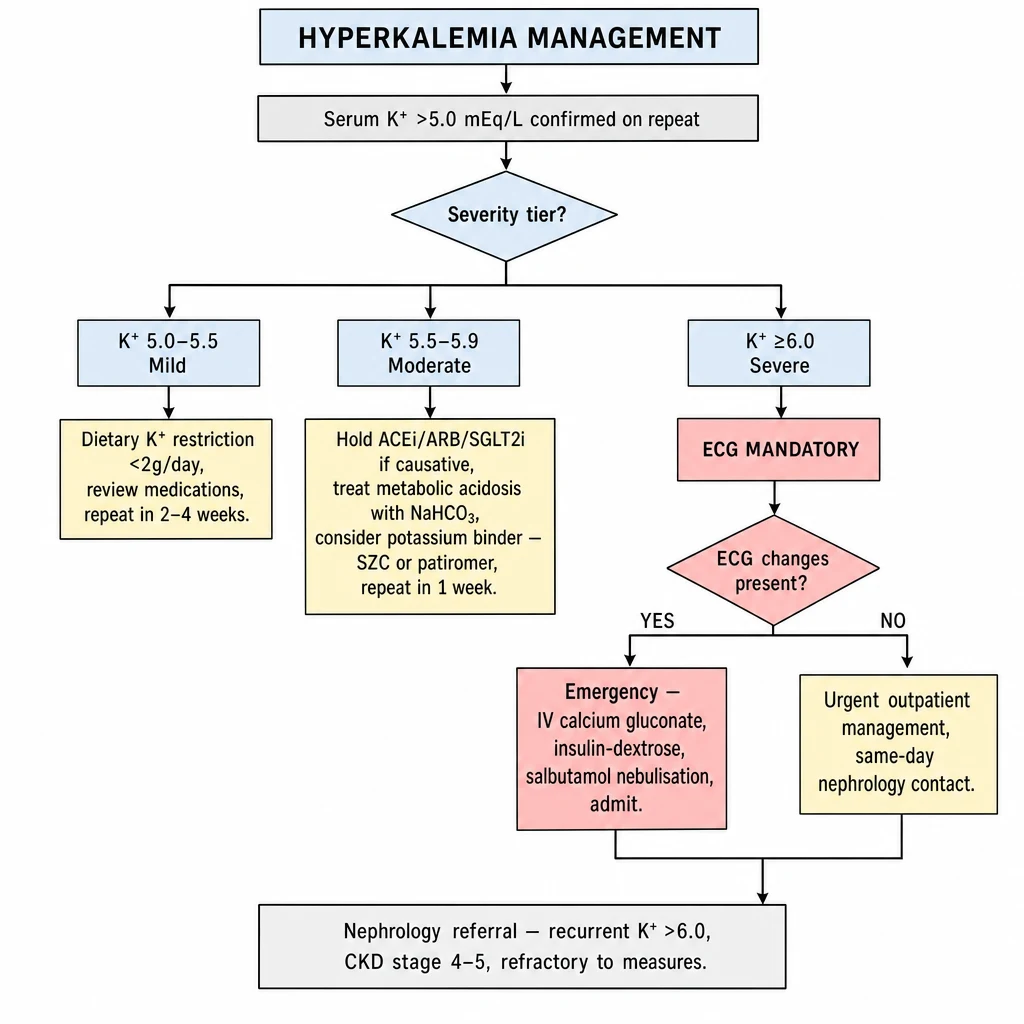 Algorithm 2 overview — Hyperkalemia Management. Classify by severity: Mild 5.0–5.5, Moderate 5.5–5.9, Severe ≥6.0 with mandatory ECG. Outpatient steps: dietary K⁺ restriction, hold offending agents, treat acidosis, consider patiromer or SZC. K⁺ ≥6.0 + ECG changes = emergency.
Algorithm 2 overview — Hyperkalemia Management. Classify by severity: Mild 5.0–5.5, Moderate 5.5–5.9, Severe ≥6.0 with mandatory ECG. Outpatient steps: dietary K⁺ restriction, hold offending agents, treat acidosis, consider patiromer or SZC. K⁺ ≥6.0 + ECG changes = emergency.
| Level | Severity | Immediate Step |
|---|---|---|
| 5.0–5.4 mEq/L | Mild | Dietary review + medication audit. Recheck in 2–4 weeks. |
| 5.5–6.0 mEq/L | Moderate | ECG. Dietary restriction. Consider potassium binder. Reduce/hold RAASi if appropriate. |
| > 6.0 mEq/L | Severe | ECG immediately. If any ECG changes → ADMIT. If ECG normal and patient asymptomatic → may manage outpatient with close follow-up. |
In-hospital: IV calcium gluconate (membrane stabilisation) → insulin + dextrose → sodium bicarbonate (if acidosis) → kayexalate/SPS enema → dialysis if refractory.
- Target <40 mEq/day (≈ 1,500 mg K⁺)
- Avoid: saging (banana), abokado (avocado), kamote, mongo, coconut water
- Leaching technique for vegetables (peel, cut, boil in large water, discard water)
- ACEi / ARB reduce dose or switch if K⁺ >5.5 with CKD
- NSAIDs stop — reduce aldosterone activity
- TMP-SMX stop — blocks ENaC like amiloride
- K-sparing diuretics hold spironolactone if K⁺ >5.5
- Loop diuretics increase dose if volume overloaded
Sodium zirconium cyclosilicate (SZC / Lokelma): 10 g TID × 48 h (acute), then 5–10 g QD maintenance. Onset 1 h. Preferred in Philippines (available). Raises serum HCO₃ slightly — beneficial in CKD acidosis.
Patiromer (Veltassa): 8.4 g QD with food. Onset 7–12 h. Not interchangeable with SZC. Use away from other medications (chelates). Limited availability in PH.
Sodium polystyrene sulphonate (Kayexalate): older agent; avoid in ileus risk; PO or enema. Still widely used in PH due to cost.
Quick Reference — Hyperkalaemia Memory Aids
- C-BIG-K⁺ Drop (acute treatment order): Calcium gluconate → Bicarbonate → Insulin+Glucose → Kayexalate/SZC → Dialysis
- Type IV RTA: low renin + low aldosterone; K⁺ 5.0–6.0; mild NAGMA; eGFR 30–60; DKD most common cause
- RAAS inhibitors: necessary for cardio-renal protection — do not stop without binder trial first
- Recheck K⁺ within 1–2 weeks after any intervention
- If on SZC: recheck K⁺ in 48–72 h during loading phase
- Avoid raw/unprocessed bananas, kamote leaves, and coconut water in dialysis patients
Hyponatremia Management
Serum Na⁺ <135 mEq/L. Classify by osmolality first, then volume status. The correction rate is as important as the target — overcorrection causes osmotic demyelination syndrome (ODS).
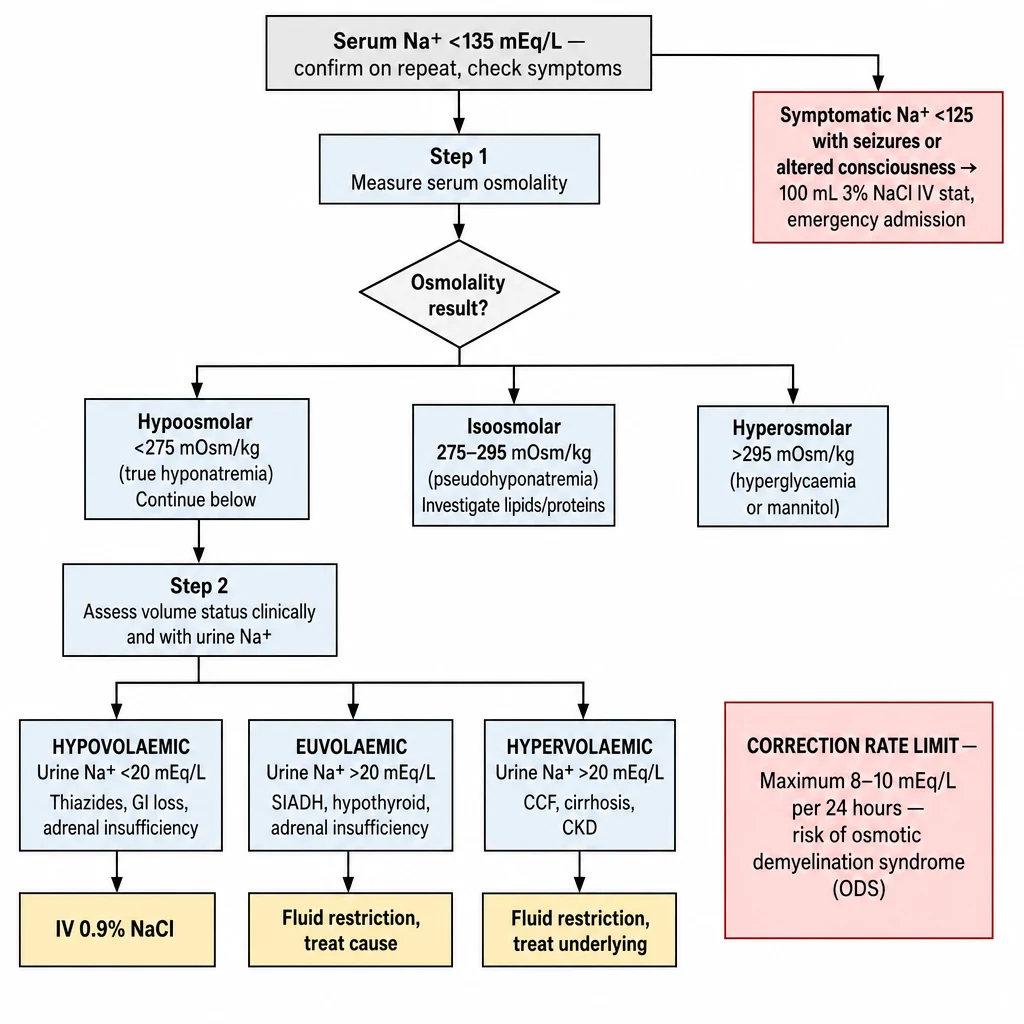 Algorithm 3 overview — Hyponatremia Management. Step 1: serum osmolality (hypoosmolar / isoosmolar / hyperosmolar). Step 2: volume status (hypovolaemic → SIADH → hypervolaemic). Step 3: correction rate — max 8–10 mEq/L per 24h to prevent ODS. Symptomatic Na⁺ <125 = 100 mL 3% NaCl bolus.
Algorithm 3 overview — Hyponatremia Management. Step 1: serum osmolality (hypoosmolar / isoosmolar / hyperosmolar). Step 2: volume status (hypovolaemic → SIADH → hypervolaemic). Step 3: correction rate — max 8–10 mEq/L per 24h to prevent ODS. Symptomatic Na⁺ <125 = 100 mL 3% NaCl bolus.
Translocational hyponatraemia. Hyperglycaemia most common. Correct Na⁺ by +1.6 mEq/L per 100 mg/dL glucose above 100. Treat glucose — Na⁺ normalises.
Pseudohyponatraemia. Extreme hyperlipidaemia or hyperproteinaemia. Measure Na⁺ on blood gas analyser (direct ISE). No treatment of Na⁺ needed.
True hyponatraemia. Proceed to Step 2: assess volume status.
- Signs: ↓ skin turgor, orthostasis, ↑ BUN/Cr ratio, dry mucosa
- Urine Na <20: extra-renal loss (vomiting, diarrhoea, burns, third-spacing)
- Urine Na >20: renal loss (diuretics, salt-wasting, Addison's)
- Treatment: Isotonic saline 0.9%. Correct volume deficit first — Na⁺ will follow.
- No edema, normal BP, mildly ↓ urine output
- SIADH most common cause
- Always rule out: hypothyroidism (TSH), cortisol deficiency (morning cortisol), medications
- Medications causing SIADH: SSRIs, SNRIs, carbamazepine, TMP-SMX, PPIs, amiodarone, cyclophosphamide, oxytocin
- Treatment: Fluid restriction 800–1,000 mL/day. Salt tabs. If refractory: tolvaptan (V2-receptor antagonist) — specialist-initiated only.
- edema + ascites present
- Causes: CHF, cirrhosis, nephrotic syndrome
- Urine Na typically <20 (effective arterial volume depletion despite edema)
- Treatment: Fluid restriction + treat underlying cause. Loop diuretic if CHF. Do not give saline.
Faster correction → Osmotic demyelination syndrome (ODS): central pontine myelinolysis. Dysarthria, dysphagia, quadriparesis, locked-in syndrome. Irreversible.
High-risk for ODS: Alcohol use disorder · malnutrition · hypokalaemia · baseline Na⁺ <120 mEq/L · liver disease.
Acute hyponatraemia (<48 h): Can correct at 1–2 mEq/L/h initially until symptoms resolve (usually +5 mEq/L sufficient for seizures/coma).
Emergency: 3% NaCl 150 mL IV over 20 min → repeat ×2 if no improvement → target +5 mEq/L in first hour → reassess. Stop 3% NaCl once symptomatic improvement or Na⁺ reaches 130 mEq/L.
SIADH Diagnostic Criteria (all must be met)
- Serum osmolality <280 mOsm/kg · Urine osmolality >100 mOsm/kg (inappropriately concentrated)
- Urine Na⁺ >40 mEq/L (renal Na wasting despite hyponatraemia) · Clinically euvolaemic
- Normal thyroid function · Normal adrenal function · Not on diuretics
- Common causes: CNS disease, pulmonary disease (TB, pneumonia, lung cancer), malignancy (SCLC), drugs
Resistant Hypertension
BP ≥ 140/90 mmHg on ≥ 3 maximally tolerated antihypertensive agents from different classes, including a diuretic. Pseudoresistance is far more common than true resistant hypertension — rule it out first.
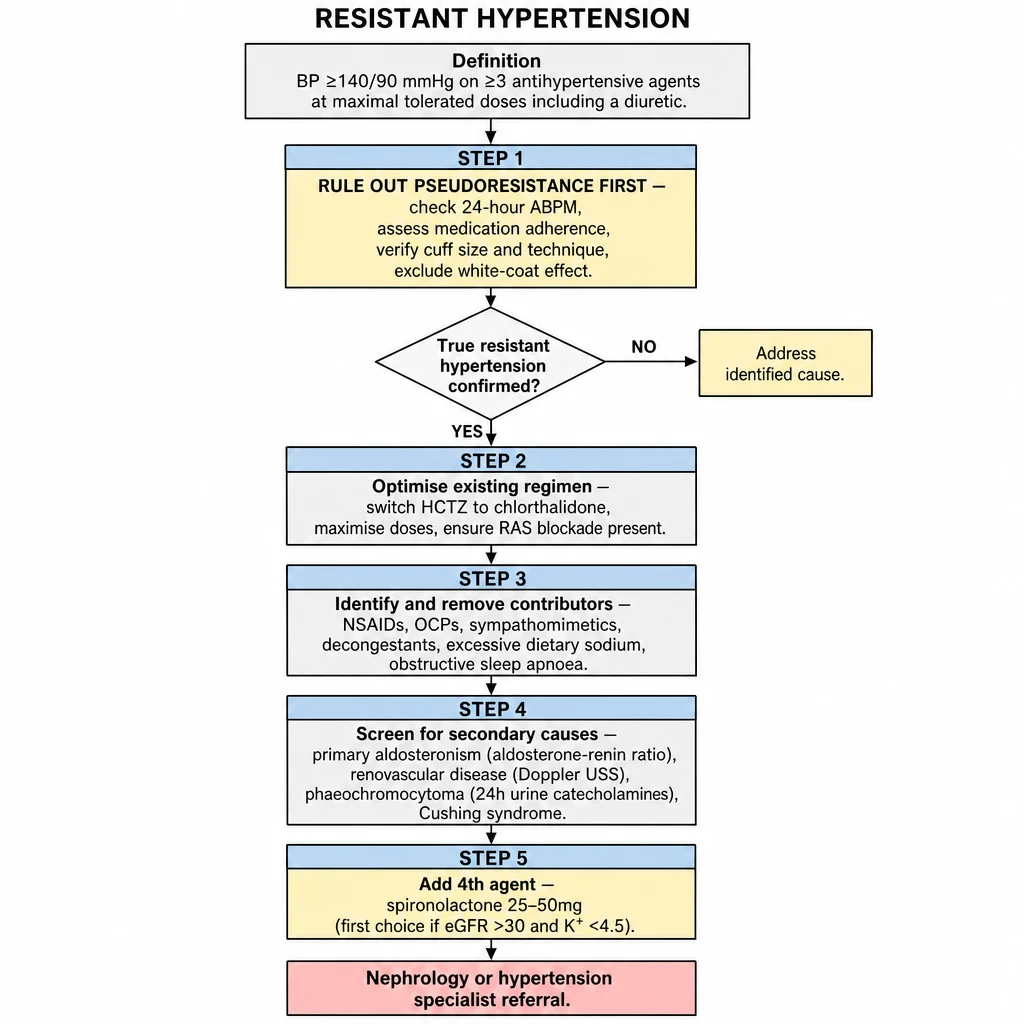 Algorithm 4 overview — Resistant Hypertension. Step 1: rule out pseudoresistance (white-coat, adherence, cuff error — check 24h ABPM). Steps 2–4: optimise regimen, screen drug/lifestyle contributors, evaluate for secondary causes. Step 5: add spironolactone 25–50 mg as preferred 4th agent.
Algorithm 4 overview — Resistant Hypertension. Step 1: rule out pseudoresistance (white-coat, adherence, cuff error — check 24h ABPM). Steps 2–4: optimise regimen, screen drug/lifestyle contributors, evaluate for secondary causes. Step 5: add spironolactone 25–50 mg as preferred 4th agent.
- Wrong cuff size (most common) — use large cuff for arm circumference >33 cm
- Talking, crossing legs, unsupported arm during measurement
- Measure after 5 min rest in seated position
- Check both arms — use higher reading arm
- White-coat HTN: Home BP monitoring (HBPM) target <135/85 mmHg at home. ABPM gold standard (daytime avg <135/85).
- Non-adherence: Pill count, pharmacy records, directly observed dosing, urine drug screen for antihypertensives (thiazide metabolite).
- Suboptimal doses or inappropriate drug combinations (two ARBs, two CCBs)
(1) Is a diuretic included? Thiazide (HCTZ/chlorthalidone) for eGFR ≥30; loop diuretic (furosemide BID) if eGFR <30 or fluid overload.
(2) Are drugs at maximum tolerated doses?
(3) Are doses timed correctly? Evening dosing of one agent improves nocturnal dipping.
(4) Single-pill combinations improve adherence — preferred where available in PH.
- Sodium intake >3 g/day (Filipino diet averages 5–6 g) — dietary recall critical
- Alcohol >14 units/week raises BP significantly
- OSA — very prevalent in PH; partner-reported snoring, BMI >30, Epworth ≥10 → sleep study
- Weight gain, sedentary lifestyle
- NSAIDs (mefenamic acid, ibuprofen) — very common in PH OTC use
- Decongestants (pseudoephedrine, phenylephrine)
- OCP (ethinylestradiol-containing pills)
- Energy drinks (caffeine + taurine)
- Corticosteroids (chronic oral prednisone)
- Calcineurin inhibitors (cyclosporine, tacrolimus)
| Cause | Prevalence | Clue | Screen |
|---|---|---|---|
| Primary hyperaldosteronism | Most common (~20%) | K⁺ low or low-normal; adrenal incidentaloma; severe or early-onset HTN | Aldosterone-to-renin ratio (ARR) — off interfering drugs ×2 weeks. ARR >30 with Aldo >15 → positive. Refer endocrine. |
| Obstructive sleep apnoea | ~30–40% | Snoring, witnessed apnoeas, daytime sleepiness, obesity, thick neck | Epworth Sleepiness Scale; overnight oximetry; polysomnography. CPAP reduces SBP ~5–10 mmHg. |
| Renal artery stenosis | ~3–5% | Flash pulmonary edema; worsening creatinine with RAASi; abdominal bruit; atherosclerotic risk; FMD (young women) | Renal Doppler USS. CTA/MRA if Doppler inconclusive. Refer vascular/nephrology. |
| Phaeochromocytoma | 0.1–0.6% | Paroxysmal headache + sweating + palpitations triad; episodic hypertension; weight loss | 24-h urine metanephrines + catecholamines (preferred) or plasma metanephrines. CT abdomen if positive. |
| Cushing's syndrome | Rare | Truncal obesity, proximal myopathy, purple striae, moon face, buffalo hump, easy bruising | Overnight 1 mg dexamethasone suppression test. Cortisol >1.8 μg/dL → positive. Refer endocrine. |
If spironolactone not tolerated (gynaecomastia, hyperkalaemia):
Eplerenone 25–50 mg (more selective, less anti-androgenic) · Doxazosin 4–8 mg (α-blocker) · Bisoprolol 5–10 mg if not on BB · Moxonidine (central α-agonist, but inferior evidence).
Avoid clonidine (rebound hypertension on missed doses — dangerous in outpatient use).
4-Drug Sequence for Resistant HTN (after pseudoresistance excluded)
- Step 1: RAS blocker (ACEi or ARB) + CCB (amlodipine) + Thiazide (chlorthalidone preferred over HCTZ) — maximise all doses
- Step 2: Add loop diuretic if eGFR <30 or edema present (switch thiazide to furosemide BID)
- Step 3: Add spironolactone 25 mg → titrate to 50 mg (PATHWAY-2 evidence)
- Step 4: Add doxazosin or bisoprolol based on patient profile · Refer if still uncontrolled
AKI Triage — Outpatient Setting
Acute Kidney Injury (KDIGO): rise in serum creatinine ≥0.3 mg/dL within 48 h, or ×1.5 baseline within 7 days, or urine output <0.5 mL/kg/h for ≥6 h. Always compare to a prior creatinine — do not assume baseline from a single elevated value.
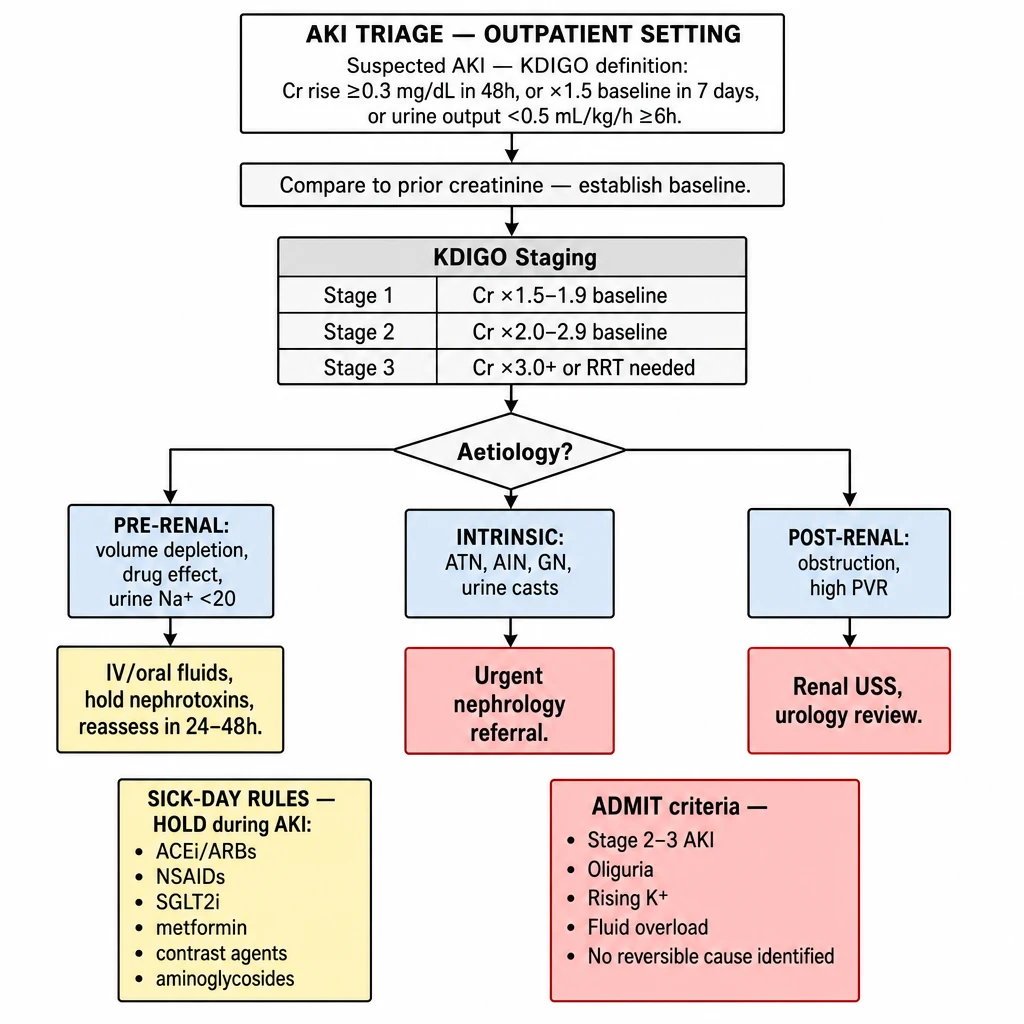 Algorithm 5 overview — AKI Triage. KDIGO staging: Stage 1 (×1.5–1.9), Stage 2 (×2.0–2.9), Stage 3 (×3.0+). Aetiologies: pre-renal (urine Na⁺ <20), intrinsic (casts, AIN, GN), post-renal (USS). Sick-day rules: hold ACEi/ARBs, NSAIDs, SGLT2i. Admit: Stage 2–3, oliguria, rising K⁺, no reversible cause.
Algorithm 5 overview — AKI Triage. KDIGO staging: Stage 1 (×1.5–1.9), Stage 2 (×2.0–2.9), Stage 3 (×3.0+). Aetiologies: pre-renal (urine Na⁺ <20), intrinsic (casts, AIN, GN), post-renal (USS). Sick-day rules: hold ACEi/ARBs, NSAIDs, SGLT2i. Admit: Stage 2–3, oliguria, rising K⁺, no reversible cause.
| Stage | Creatinine criterion | Urine output | Typical approach |
|---|---|---|---|
| Stage 1 | ×1.5–1.9 baseline or ↑ ≥0.3 mg/dL | <0.5 mL/kg/h × 6–12 h | Outpatient if pre-renal likely; remove offending agents; 48 h recheck |
| Stage 2 | ×2.0–2.9 baseline | <0.5 mL/kg/h × 12 h | Strong consideration for admission; close monitoring at minimum |
| Stage 3 | ×3.0 or Cr >4.0 mg/dL or initiation of KRT | <0.3 mL/kg/h × 24 h or anuria × 12 h | Admit — nephrology consult urgent |
- History: vomiting, diarrhoea, poor oral intake, bleeding, diuretic use, heat exposure
- Exam: decreased turgor, orthostasis (↑ HR or ↓ SBP ≥20 on standing), dry mucosa
- Labs: BUN/Cr >20 · FENa <1% (unreliable if on diuretics — use FEUrea <35% instead) · Urine SG >1.020
- Treatment: Oral/IV rehydration. Stop NSAIDs, diuretics. Hold ACEi/ARB temporarily.
- ATN: Recent contrast, aminoglycosides (amikacin), prolonged pre-renal, rhabdomyolysis (CPK elevation)
- GN: Active urine sediment (dysmorphic RBCs, RBC casts), proteinuria, hematuria, hypertension, systemic symptoms (rash, arthralgias, haemoptysis)
- AIN: Recent drug (NSAIDs, PPIs — especially high-dose, beta-lactam antibiotics) · rash + eosinophilia + fever (Triad present in only 10%) · FENa >1%
- Classic: BPH (most common in Filipino men >60), bladder neck obstruction, pelvic malignancy, bilateral ureteric stones, neurogenic bladder
- Exam: palpable bladder, suprapubic fullness, flank pain
- Test: Bedside bladder USS (post-void residual >300 mL) or renal USS (hydronephrosis bilateral). Relief of obstruction often restores function rapidly.
ACEi / ARB — hold if volume depleted, K⁺ >5.5, or creatinine rising >25% within 2 weeks of initiation
Metformin — hold if Cr >1.5 mg/dL in women, >1.7 in men, or any AKI (lactic acidosis risk)
SGLT2 inhibitors — hold during any acute illness / hospitalisation (euglycaemic DKA risk)
Contrast agents — schedule IV contrast procedures only when renal function stable
Aminoglycosides — adjust dose per eGFR; avoid in AKI unless no alternative
Beta-blockers — continue; do not stop abruptly
Statins — continue
Outpatient AKI Monitoring Plan (Stage 1 Pre-renal — safe for outpatient)
- Remove offending agents (NSAIDs, diuretics, RAASi temporarily)
- Oral rehydration: 2–2.5 L oral fluids per day if not contraindicated by cardiac status
- Recheck creatinine, electrolytes, and urine output assessment in 48–72 h
- Clear return precautions: ↓ urine output, worsening edema, confusion, chest pain, BP >180/120
- If not improving or worsening at 48-h recheck → escalate to admission
On diuretics? Add BUN values to calculate FeUrea (more reliable):
CKD Referral Thresholds
Based on KDIGO 2024 CKD guidelines. Referral is based on eGFR, albuminuria, rate of decline, and complications — not eGFR alone. Many patients with eGFR 45–60 can be safely managed in primary care with shared-care guidance.
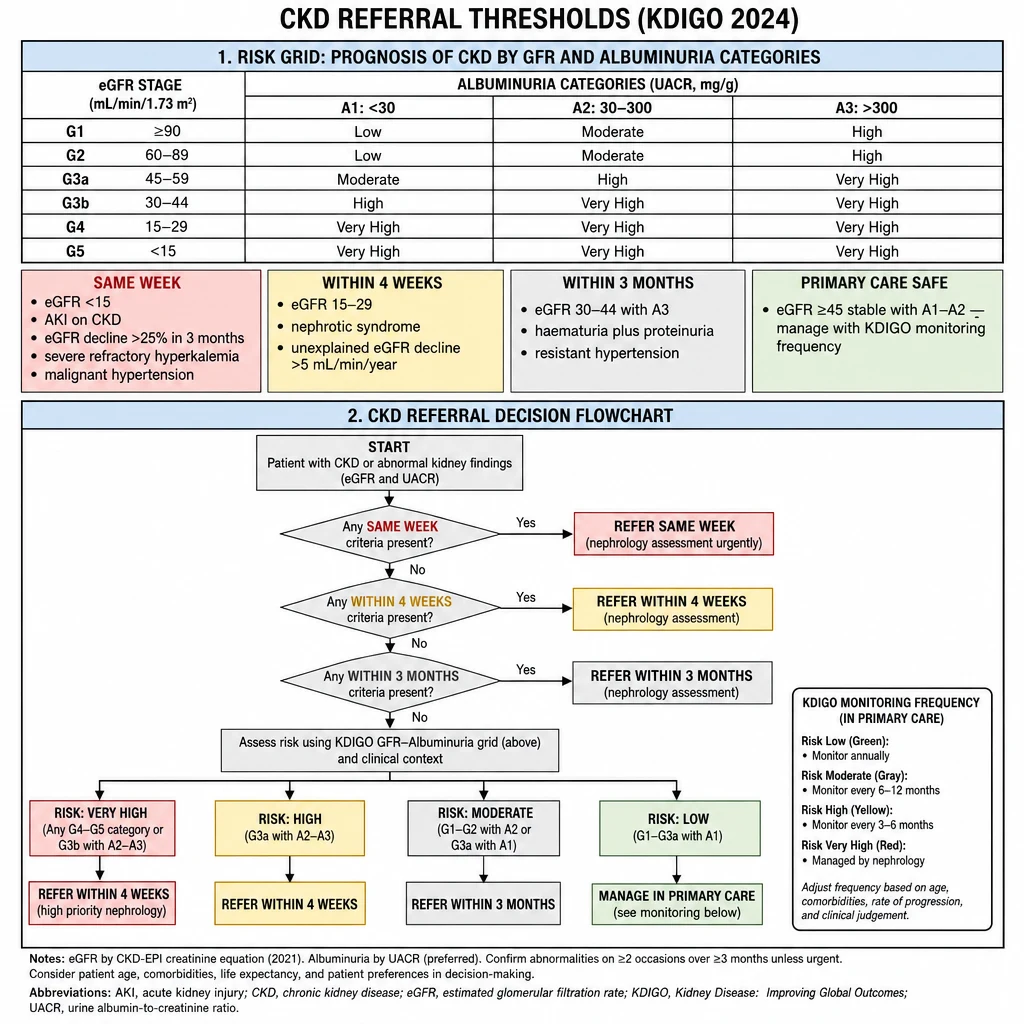 Algorithm 6 overview — CKD Referral Thresholds (KDIGO 2024). The G×A heat-map assigns green / yellow / amber / red risk. Urgency tiers: Same week (eGFR <15, AKI-on-CKD, malignant HTN) → 4 weeks (eGFR 15–29, nephrotic) → 3 months (eGFR 30–44 + A3) → Primary care safe (eGFR ≥45 stable, A1–A2).
Algorithm 6 overview — CKD Referral Thresholds (KDIGO 2024). The G×A heat-map assigns green / yellow / amber / red risk. Urgency tiers: Same week (eGFR <15, AKI-on-CKD, malignant HTN) → 4 weeks (eGFR 15–29, nephrotic) → 3 months (eGFR 30–44 + A3) → Primary care safe (eGFR ≥45 stable, A1–A2).
Suspected rapidly progressive GN: hematuria + proteinuria + creatinine rising over weeks (RPGN may progress to dialysis-dependence within weeks if untreated)
Hyperkalaemia >6.5 mEq/L not responding to emergency measures
Hypertensive emergency with new renal impairment
Pulmonary edema with new oliguria
Suspected hemolytic uraemic syndrome (microangiopathic hemolytic anemia + thrombocytopaenia + AKI)
eGFR decline >5 mL/min/1.73m²/year (rapid progressor) or >10 mL/min in 5 years
Persistent urine ACR >300 mg/g despite optimised ACEi/ARB + BP control
Recurrent AKI episodes (>3 per year)
Difficult-to-manage HTN with CKD (suspected renovascular or secondary cause)
Inherited kidney disease: PKD, Alport syndrome, FSGS in young patient
Unexplained proteinuria >1 g/g without diabetes or HTN
Diabetic nephropathy G3a+ with ACR >300 despite maximal dual RAS blockade
CKD with suspected glomerular disease (hematuria + proteinuria, abnormal sediment)
CKD requiring biopsy for diagnosis (proteinuria without clear cause)
Review frequency by G×A risk category: Low (G1–G2, A1) = annual; Moderate (G3a, A1) = annual; High (G3a A2, G3b A1) = 2×/year; Very High = 3–4×/year
Monitor: BP, eGFR, ACR, electrolytes (K⁺, HCO₃), Hgb, Ca, PO₄, PTH (if eGFR <45)
Rule of thumb: Refer when you would question your next step
- eGFR <30 → always refer (G4/G5)
- ACR >300 persistent → always refer
- Rapidly declining eGFR → always refer
- Any doubt about aetiology → refer for biopsy consideration
- AVF planning: Refer vascular surgery when eGFR <25 and HD is likely trajectory — earlier creation means better maturation
- Pre-dialysis education: Start when eGFR <30 — modality choice, diet, access, transplant evaluation
- Transplant referral: eGFR <20 and declining — pre-emptive transplant is the best option
CKD anemia Workflow
anemia of CKD is a diagnosis of exclusion — always rule out iron deficiency, hemolysis, B12/folate deficiency, and GI blood loss before attributing anemia to EPO deficiency. The sequence: replete iron → reassess → consider ESA.
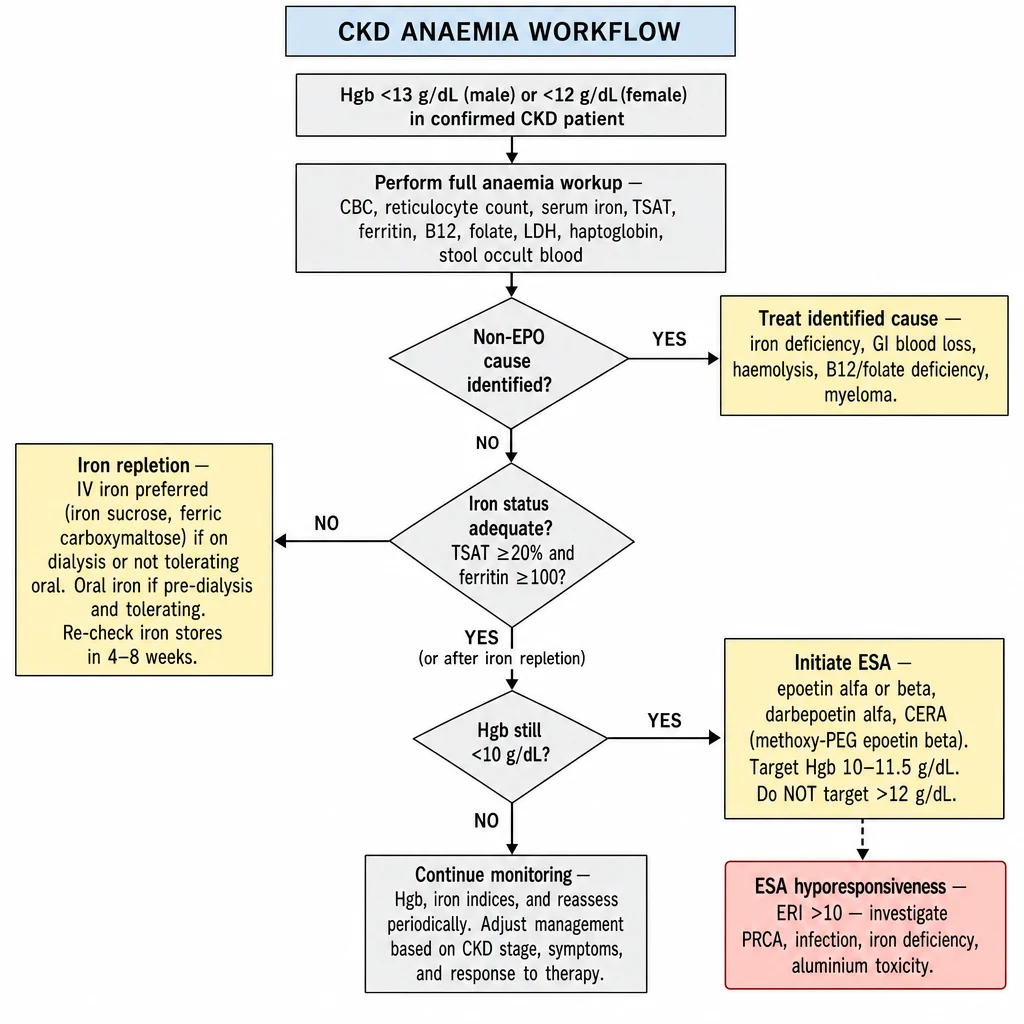 Algorithm 7 overview — CKD anemia Workflow. Workup first: CBC, iron studies, reticulocytes, B12/folate, LDH, stool OB. Rule out non-EPO causes. Iron repletion (IV preferred): TSAT <20% or ferritin <100. If Hgb still <10 after iron → ESA (epoetin, darbepoetin, CERA). Target Hgb 10–11.5 g/dL. ERI >10 = investigate hyporesponsiveness.
Algorithm 7 overview — CKD anemia Workflow. Workup first: CBC, iron studies, reticulocytes, B12/folate, LDH, stool OB. Rule out non-EPO causes. Iron repletion (IV preferred): TSAT <20% or ferritin <100. If Hgb still <10 after iron → ESA (epoetin, darbepoetin, CERA). Target Hgb 10–11.5 g/dL. ERI >10 = investigate hyporesponsiveness.
Vitamin B12 · Folate · LDH + haptoglobin + peripheral smear (hemolysis screen)
Faecal occult blood test (GI blood loss) · Stool H. pylori (common cause of iron deficiency in PH)
If hemolysis suspected: Direct Coombs, G6PD deficiency screen
| Population | Iron deficient if | Treatment |
|---|---|---|
| CKD non-dialysis | Ferritin <100 ng/mL or TSAT <20% | Oral iron first-line |
| CKD on HD | Ferritin <200 ng/mL or TSAT <20% | IV iron preferred (poor oral absorption, inflammation) |
| CKD on PD | Ferritin <100 ng/mL or TSAT <20% | Oral or IV iron |
IV iron options (available in PH): Iron sucrose (Venofer) 200 mg over 30 min × 5 doses · Ferric carboxymaltose (Ferinject) 500–1000 mg single infusion (off-label in CKD; widely used)
Recheck iron stores at 3 months. A Hgb response of ≥1 g/dL in 4–6 weeks confirms iron-responsive anemia.
- Target Hgb: 10–11.5 g/dL (KDIGO 2024 — do NOT target >13 g/dL: ↑CVD risk, stroke)
- ESA options (PH): EPO-alfa (Eprex) 50–100 IU/kg SC 3×/week · Darbepoetin-alfa 0.45 mcg/kg SC Q2W · EPO-beta (NeoRecormon)
- Check reticulocyte response at 2–4 weeks. Titrate dose by 25–50% if Hgb not rising.
- Do not use ESA if active malignancy (promotes tumour growth), uncontrolled HTN, or pure red cell aplasia
Iron-responsive anemia corrected. Recheck Hgb every 3 months. Maintain TSAT >20% and ferritin >100. Continue oral iron maintenance if oral route tolerated.
Common causes: Iron deficiency (most common — recheck stores) · Active infection or inflammation (hepcidin ↑) · Hyperparathyroidism (PTH >500 suppresses erythropoiesis) · Folate/B12 deficiency · Aluminium toxicity (rare) · Dialysis inadequacy (Kt/V <1.2) · Pure red cell aplasia (anti-EPO antibodies — check if on IV EPO >3 months with sudden resistance)
Consider transfusion if: Hgb <7 g/dL with symptoms (dyspnoea at rest, angina, altered sensorium) · Hgb <8 g/dL peri-operatively · Acute hemorrhage requiring immediate correction.
If transfusion required in transplant candidate → document, inform transplant team, request leuco-depleted filtered blood.
CKD anemia Targets — KDIGO 2024
- Target Hgb:
10.0–11.5 g/dLfor most CKD patients on ESA - Do NOT target Hgb >13 g/dL — TREAT (normal Hgb trial): ↑ stroke, thromboembolic events, death
- Iron target: TSAT
≥20%+ Ferritin>100 ng/mL(non-dialysis) or>200(HD) - Do not give IV iron if ferritin >500 (functional iron overload risk) without reassessment
- HIF-PHI (roxadustat, daprodustat): approved in some countries; monitor CVD risk; check local availability in PH
Proteinuria Workup
Proteinuria on dipstick must be confirmed quantitatively and be persistent (≥2 readings ≥3 months apart) to diagnose CKD. The degree and pattern guide the diagnostic pathway.
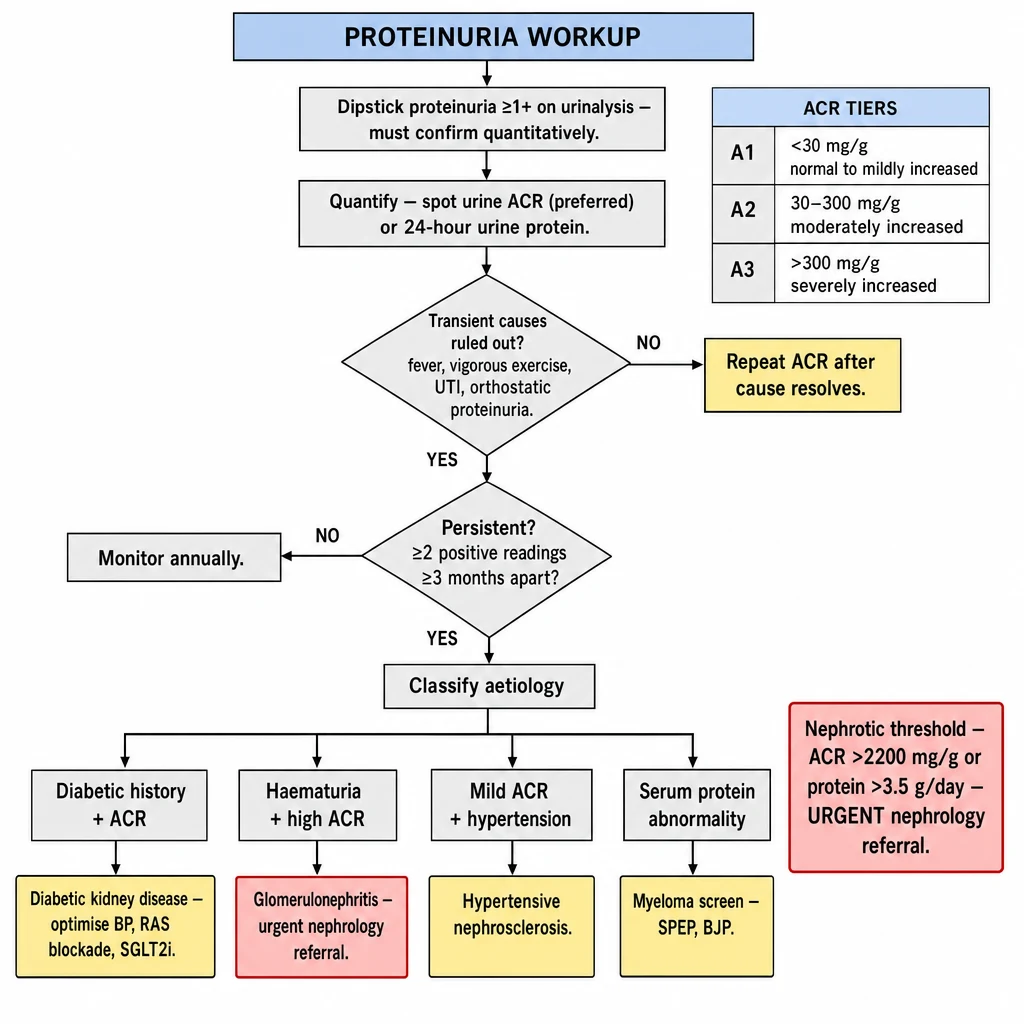 Algorithm 8 overview — Proteinuria Workup. Quantify: spot urine ACR (A1 <30 / A2 30–300 / A3 >300 mg/g). Rule out transient causes (fever, exercise, UTI, orthostatic). Persistent = ≥2 readings over 3 months. Aetiology: DKD, hypertensive nephrosclerosis, GN, myeloma (BJP). Nephrotic threshold ACR >2200 mg/g = urgent nephrology referral.
Algorithm 8 overview — Proteinuria Workup. Quantify: spot urine ACR (A1 <30 / A2 30–300 / A3 >300 mg/g). Rule out transient causes (fever, exercise, UTI, orthostatic). Persistent = ≥2 readings over 3 months. Aetiology: DKD, hypertensive nephrosclerosis, GN, myeloma (BJP). Nephrotic threshold ACR >2200 mg/g = urgent nephrology referral.
Confirm with: Spot urine albumin-to-creatinine ratio (ACR) — preferred, most practical in PH outpatient setting. Alternatively, 24-hour urine protein collection (gold standard but cumbersome).
| ACR mg/g (or mg/mmol) | Category | Clinical Significance |
|---|---|---|
| <30 mg/g | A1 — Normal / mildly increased | Monitor annually if CKD risk factors present |
| 30–300 mg/g | A2 — Moderately increased | Microalbuminuria — CKD marker; maximise ACEi/ARB + SGLT2i |
| >300 mg/g | A3 — Severely increased | Macroalbuminuria — refer nephrology; high progression and CVD risk |
| >2,200 mg/g | Nephrotic range | Evaluate for nephrotic syndrome — urgent nephrology referral |
Orthostatic proteinuria: Common in adolescents and young adults. Protein present only in upright urine; absent in first morning void (supine overnight). Benign; confirm with split urine collection.
Reassure. Repeat ACR in 6–12 months. No treatment needed. If ACR normalises and remains normal — not CKD.
Classify aetiology and determine CKD stage with eGFR. Proceed with workup below.
- Diabetes + ACR 30–300 (microalbuminuria) + NO hematuria + eGFR may be normal or ↓
- Typically gradual onset; bilateral kidneys normal size or enlarged
- Management: ACEi or ARB (first-line) · SGLT2i (canagliflozin, empagliflozin) · BP <130/80 · HbA1c <7% · Finerenone if ACR >300 + eGFR 25–75
- Refer if ACR >300 or eGFR declining despite optimised therapy
- Check: ANA, anti-dsDNA (lupus) · ANCA (vasculitis) · C3/C4 (complement-mediated) · Anti-PLA2R (MN) · SPEP/UPEP (myeloma if >40 y/o) · Hepatitis B/C serology · HIV
- Active urine sediment (RBC casts, dysmorphic RBCs) → GN → urgent nephrology
- Heavy proteinuria + normal urine sediment → membranous nephropathy or FSGS → refer
Causes in Filipino adults: Membranous nephropathy (most common adult-onset) · FSGS · Minimal change disease (often steroid-responsive) · Amyloidosis (if myeloma, chronic infection, or FMF) · Diabetic nephropathy (if heavy).
Complications to manage while awaiting nephrology: Thromboembolism (PE risk when albumin <2.0 — consider anticoagulation) · Infection risk (encapsulated organisms — vaccinate) · Hyperlipidaemia (statin).
Proteinuria Workup Summary — Outpatient Approach
- Confirm: Repeat spot ACR × 2 readings, ≥3 months apart
- Quantify: ACR (spot) or 24-h urine protein (if ACR inconclusive)
- Characterise: Urine microscopy (casts, dysmorphic RBCs?)
- Baseline: eGFR, electrolytes, albumin, LFTs, CBC, BP
- Diabetic: ACEi/ARB + SGLT2i + BP control → refer if ACR >300 or declining
- Non-diabetic + hematuria + casts → GN → urgent nephrology
- Nephrotic range → always refer → biopsy usually required
- ACR 30–300 stable + diabetes/HTN controlled → manage in primary care
Metabolic Acidosis Correction
Step-wise approach: confirm the primary disorder, calculate the anion gap (with albumin correction), classify, then treat the cause. CKD metabolic acidosis (Type IV RTA and uraemic acidosis) are the most common outpatient presentations.
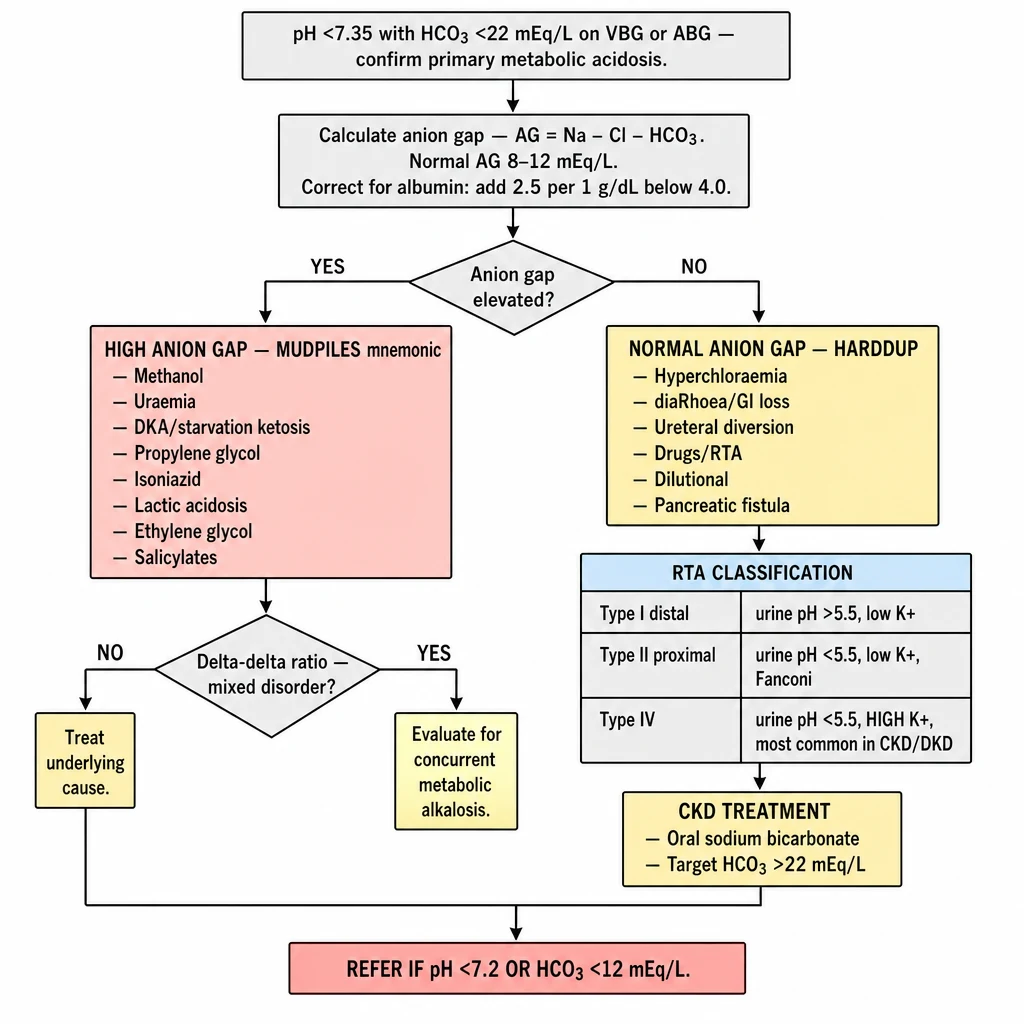 Algorithm 9 overview — Metabolic Acidosis. Confirm: pH <7.35, HCO₃ <22. Calculate AG (Na − Cl − HCO₃; correct for albumin). High AG (MUDPILES): uremia, DKA, lactic acidosis, toxins. Normal AG (HARDDUP): hyperchloraemic — RTA types I/II/IV, diarrhoea. CKD treatment: oral NaHCO₃, target HCO₃ >22. Refer if pH <7.2.
Algorithm 9 overview — Metabolic Acidosis. Confirm: pH <7.35, HCO₃ <22. Calculate AG (Na − Cl − HCO₃; correct for albumin). High AG (MUDPILES): uremia, DKA, lactic acidosis, toxins. Normal AG (HARDDUP): hyperchloraemic — RTA types I/II/IV, diarrhoea. CKD treatment: oral NaHCO₃, target HCO₃ >22. Refer if pH <7.2.
Winter's formula (expected pCO₂ for pure metabolic acidosis):
MUDPILES mnemonic:
- Methanol poisoning
- Uraemia (CKD G4–G5)
- DKA / alcoholic / starvation ketoacidosis
- Propylene glycol (IV medications)
- Isoniazid / Iron toxicity
- Lactic acidosis (Type A: hypoperfusion; Type B: metformin, liver disease)
- Ethylene glycol (antifreeze)
- Salicylate toxicity
Calculate osmolar gap if toxic alcohol suspected: OG = measured Osm − calculated Osm. OG >10 → toxic alcohol.
Calculate urine anion gap (UAG):
- Negative UAG (−): Appropriate NH₄⁺ excretion. Extra-renal cause: diarrhoea (most common in PH), ileostomy, fistula. → Treat with oral NaHCO₃ or K-citrate.
- Positive UAG (+): Impaired NH₄⁺ excretion → Renal tubular acidosis (RTA).
| Type | Urine pH | K⁺ | HCO₃ | Cause | Action |
|---|---|---|---|---|---|
| Type I (Distal) | >5.5 (can't acidify) | Low | Variable (often <15) | Sjögren's, autoimmune, amphotericin, nephrocalcinosis/stones | NaHCO₃ or K-citrate. Refer nephrology. |
| Type II (Proximal) | <5.5 (can acidify, but leaks HCO₃) | Low | <15 mEq/L | Fanconi syndrome, myeloma, tenofovir, heavy metals | High-dose NaHCO₃ (often 10+ mEq/kg/day). Refer nephrology. |
| Type IV (Hypoaldosteronism) | <5.5 | High | Mild reduction (18–22) | Most common in CKD/DKD, ACEi/ARB use — hyporeninaemic hypoaldosteronism | Treat hyperkalaemia (Algorithm 2). Fludrocortisone if confirmed Addison's. Often improves with NaHCO₃ + K⁺ management. |
Sodium bicarbonate (NaHCO₃):
Starting dose: 0.5–1.0 mEq/kg/day divided into 2–3 doses with meals
Tablet: NaHCO₃ 650 mg = 7.7 mEq HCO₃ (available in PH pharmacies)
Powder: Baking soda (sodium bicarbonate) 1 level teaspoon = 48 mEq — practical and inexpensive for PH patients
Titrate every 4 weeks until HCO₃ reaches 22–26 mEq/L
Caution with sodium load: Each gram NaHCO₃ = 12 mEq Na⁺ — monitor BP and edema. If fluid overload is a concern, consider potassium citrate (if K⁺ is normal or low) as a sodium-free alternative.
Benefits beyond acidosis correction: Improved muscle protein retention · Reduced phosphate release from bone · Better response to EPO · Reduced hyperkalaemia (see Algorithm 2)
Quick Reference — Metabolic Acidosis Formulas
- Anion gap:
Na − (Cl + HCO₃)· Normal 8–12 mEq/L - Albumin correction:
AG + 2.5 × (4 − Alb) - Winter's formula:
pCO₂ = (1.5 × HCO₃) + 8 ± 2 - Delta-delta:
(AG−12) / (24−HCO₃)
- Urine AG:
UNa + UK − UCl· Negative = GI loss · Positive = RTA - NaHCO₃ 650 mg tab =
7.7 mEqHCO₃ - Baking soda 1 tsp =
~48 mEqNaHCO₃ (practical for home use) - Type IV RTA = most common CKD acidosis; hyperkalemia + mild NAGMA in DKD
